Orthodontic Headgear
Sometimes, braces alone aren’t enough to move teeth into a better position, or to correct trouble with the bite or remedy problems in the growth of the jaws. In those situations, special appliances may be recommended. Orthodontic headgear is the general name for an appliance, worn partly outside the mouth, which creates just enough force to move the teeth properly and guide the growth of the face and jaws.
There are several different types of orthodontic headgear, each designed to work best in a specific situation. A treatment program will be designed to address your individual needs, and select the most appropriate type of headgear; you will also be instructed on its use and care. It’s important for you to follow instructions carefully so that you can achieve the best results from your treatment.
Types of Headgear
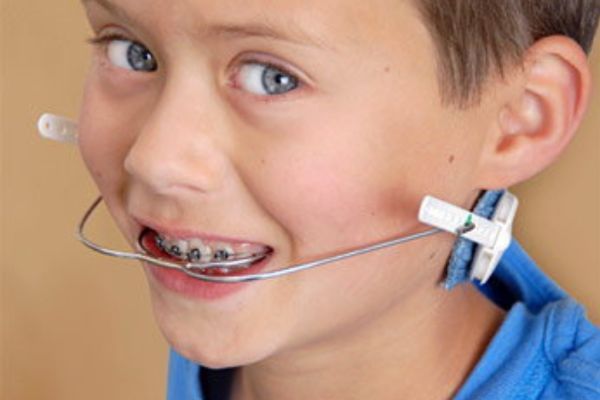
One common type of headgear is called the cervical pull type. This appliance has a U- shaped wire that attaches to the bands on your back teeth, and a strap that is worn behind your neck. A similar device is the high-pull headgear, which also has a wire connecting to the teeth, plus a strap that goes behind and over the head.
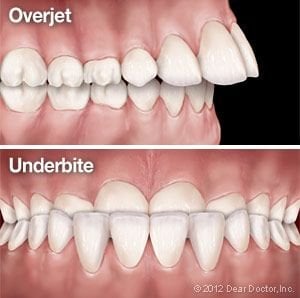
These types of headgear are typically used to correct an excessive horizontal overbite (technically called an “overjet”) in children, by holding back the growth of the upper jaw. They can also be used for adults who need help maintaining a proper bite and correct tooth spacing after tooth extraction. Generally, these types of headgear are designed to be worn from 12-14 hours each day.
Another type of headgear is the reverse-pull or “facemask” type. This appliance is generally used to correct an underbite. It gently pulls the upper jaw forward (instead of back), which allows it to catch up with the lower jaw. It consists of two pads — one resting on the forehead, the other on the chin — connected by a vertical frame. Elastics or wires, which connect from the frame to the braces, exert the pulling force. It may be necessary to wear this appliance from 14-16 hours daily.
Making Headgear Work Depends on You
Whichever type of headgear you’re wearing, there are some important things you should know. Probably the most essential one is this: In order for it to be effective, you must carefully follow instructions about wearing your headgear — that means putting it on each day for the time specified. If you wear headgear at night and you miss one night, you must make up the time the following day — otherwise, everything you’ve accomplished in the previous seven days of wear could be wiped out!
It’s normal to feel some discomfort as you get used to wearing orthodontic headgear. Fortunately, if you wear it faithfully, the discomfort generally goes away in a few days. An over-the-counter pain reliever like Ibuprofen, and/or a soft diet, may be recommended to help you adjust.
From time to time you may also experience some soreness when chewing, or even a little looseness in the first molars. This is normal, and it shows the appliance is working. However, if you have unusual pain, notice that the anchor band on your first molar (the one the headgear attaches to) has come loose, or find that the headgear suddenly seems not to fit correctly, it could signal a problem that requires immediate attention.
Maintain Your Headgear — And Your Oral Health
To keep your orthodontic headgear working as it should — and to maintain your overall oral health — it’s important that you follow all instructions about care and cleaning. It’s also important that you learn to put headgear on and take it off properly and safely. Remember to bring it with you every time you have an orthodontic appointment — but leave it behind when you’re playing sports, or even horsing around in the living room!
Wearing orthodontic headgear may seem like a big adjustment — and nobody would deny that it takes some getting used to. When everyone works together, it’s possible to achieve your goal: a beautiful smile that you’ll have for your whole lifetime.





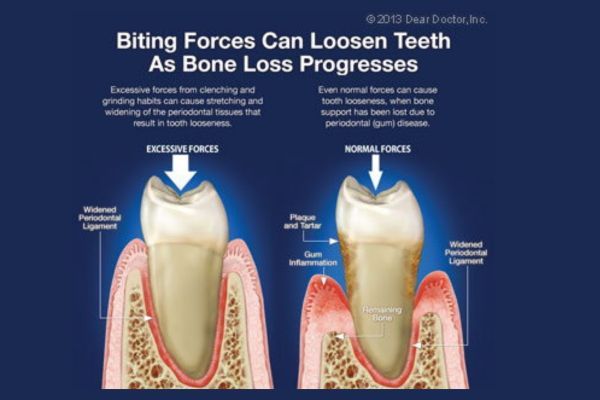
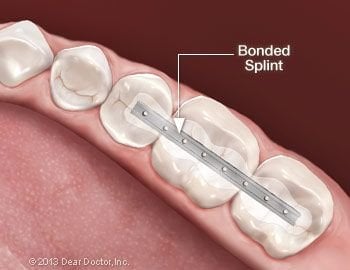 It is also possible to reduce stresses on teeth by temporarily or permanently splinting them together like fence pickets so that any biting force is distributed among groups of teeth rather than individual loosened teeth. The splint is a very small metal bracket bonded to the backs of or tops of the teeth.
It is also possible to reduce stresses on teeth by temporarily or permanently splinting them together like fence pickets so that any biting force is distributed among groups of teeth rather than individual loosened teeth. The splint is a very small metal bracket bonded to the backs of or tops of the teeth.
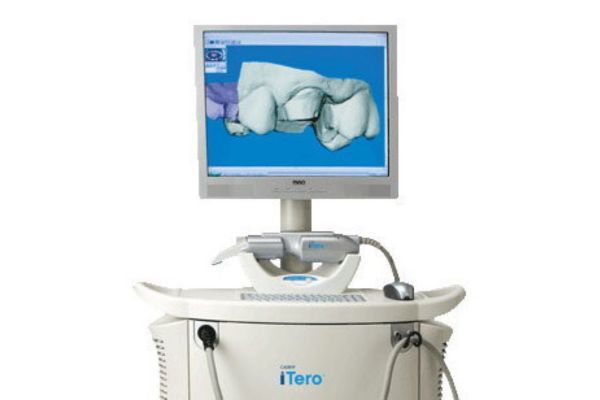
 This remarkable tool uses blue wavelength light to precisely capture the unique nooks and crannies of your tooth’s surface and make a highly accurate 3D digital model. It makes it possible to instantaneously examine your tooth, and your bite. It’s possible to identify any additional prep work required for new crowns, veneers and fillings right then and there; to implement any needed changes; and to rescan the tooth to create a new series of images and 3D model.
This remarkable tool uses blue wavelength light to precisely capture the unique nooks and crannies of your tooth’s surface and make a highly accurate 3D digital model. It makes it possible to instantaneously examine your tooth, and your bite. It’s possible to identify any additional prep work required for new crowns, veneers and fillings right then and there; to implement any needed changes; and to rescan the tooth to create a new series of images and 3D model.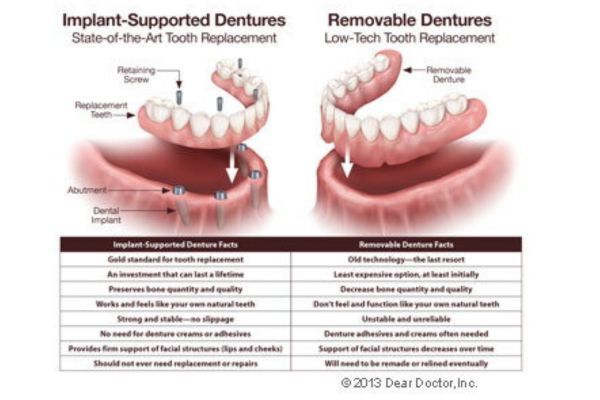
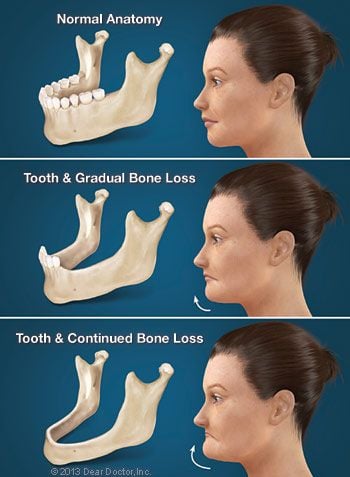
 The surgery to place dental implants that support a fixed denture is a simple, routine procedure carried out in an office setting, under local anesthesia in most cases. (If you need to have failing teeth removed, that will be done first, often the same day your implants are placed). After numbing the area, the appropriate number of implants will be placed in your jaw at precisely planned angles and positions to maximize support and avoid anatomical structures such as nerves and sinuses. Depending on how many implants are needed, the surgery can take anywhere from one to three hours. Most people who have dental implants placed find that any post-operative discomfort can be managed with over-the-counter anti-inflammatory medication such as ibuprofen or acetaminophen. Some don’t even need to take that.
The surgery to place dental implants that support a fixed denture is a simple, routine procedure carried out in an office setting, under local anesthesia in most cases. (If you need to have failing teeth removed, that will be done first, often the same day your implants are placed). After numbing the area, the appropriate number of implants will be placed in your jaw at precisely planned angles and positions to maximize support and avoid anatomical structures such as nerves and sinuses. Depending on how many implants are needed, the surgery can take anywhere from one to three hours. Most people who have dental implants placed find that any post-operative discomfort can be managed with over-the-counter anti-inflammatory medication such as ibuprofen or acetaminophen. Some don’t even need to take that.

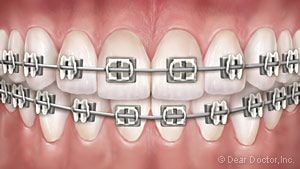 Metal Braces need no introduction. But you might be surprised to find they’re smaller and lighter than ever. They may even offer some customized options, like colored elastic ties on the brackets.
Metal Braces need no introduction. But you might be surprised to find they’re smaller and lighter than ever. They may even offer some customized options, like colored elastic ties on the brackets.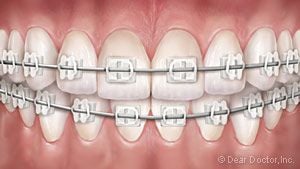 Clear Braces feature brackets made of ceramic or composite materials which blend in with your teeth, making them harder to notice. They’re suitable in many situations, but they cost a little more.
Clear Braces feature brackets made of ceramic or composite materials which blend in with your teeth, making them harder to notice. They’re suitable in many situations, but they cost a little more.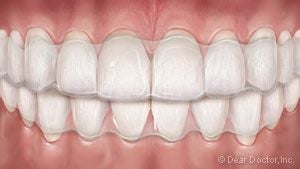 Clear Aligners for teens is a series of removable, clear plastic trays that gradually straighten teeth as they’re worn (for 22 hours per day). Formerly recommended only for adult patients, they now come with special features — like compliance indicators to tell how often you’ve been wearing them — that make them appropriate for teens in some situations. The advantage: they’re practically invisible!
Clear Aligners for teens is a series of removable, clear plastic trays that gradually straighten teeth as they’re worn (for 22 hours per day). Formerly recommended only for adult patients, they now come with special features — like compliance indicators to tell how often you’ve been wearing them — that make them appropriate for teens in some situations. The advantage: they’re practically invisible!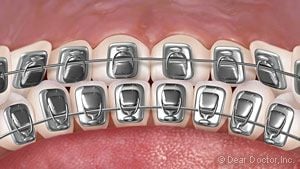 Lingual Braces offer the most unnoticeable form of orthodontic treatment because they are attached to the back (tongue side) of the teeth, where they cannot be seen at all.
Lingual Braces offer the most unnoticeable form of orthodontic treatment because they are attached to the back (tongue side) of the teeth, where they cannot be seen at all.