Fluoride & Your Child
Fluoride, a naturally occurring mineral, is essential for proper tooth development and the prevention of tooth decay. In communities throughout the United States, tooth decay may still be a significant problem — but it is far less prevalent than it would have been, if not for the fluoridation of public water supplies. That’s why the major associations of pediatric dentists and doctors support water fluoridation to the current recommended levels of 0.70 parts per million (ppm). It’s also why the federal Centers for Disease Control and Prevention (CDC) has called fluoridated water one of the most significant health achievements of the 20th century.
Of course, not everyone has access to fluoridated water. That’s one reason why a fluoride supplement is often recommended for your child and/or the use of toothpastes and other products that contain this important mineral. Because it is possible for children to get too much fluoride, it is best to seek professional advice on the use of any fluoride-containing product.
How Fluoride Helps
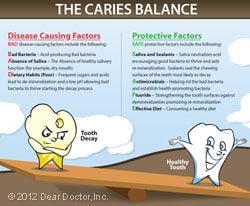
The protective outer layer of teeth, called enamel, is often subject to attacks from acids. These can come directly from acidic foods and beverages, such as sodas and citrus fruits — or sometimes through a middleman: the decay-causing bacteria already in the mouth that create acid from sugar. These bacteria congregate in dental plaque and feed on sugar that is not cleansed from your child’s mouth. In metabolizing (breaking down) sugar, the bacteria produce acids that can eat through tooth enamel. This is how cavities are formed. When fluoride is present, it becomes part of the crystalline structure of tooth enamel, hardening it and making it more resistant to acid attack. Fluoride can even help repair small cavities that are already forming.
Delivering Fluoride to the Teeth
Fluoride ingested by children in drinking water or supplements can be taken up by their developing permanent teeth. Once a tooth has erupted, it can be strengthened by fluoride topically (on the surface). Using a fluoride-containing toothpaste is one way to make sure your children’s teeth receive helpful fluoride exposure daily. We recommend using only a pea-sized amount for children ages 2-6 and just a tiny smear for kids under two. Fluoride should not be used on children younger than six months. A very beneficial way to deliver fluoride to the teeth is with topical fluoride applications painted right onto your child’s teeth and allowed to sit for a few minutes for maximum effectiveness.
How Much Is Too Much?
Teeth that are over-exposed to fluoride as they are forming beneath the gum line can develop a condition called enamel fluorosis, which is characterized by a streaked or mottled appearance. Mild fluorosis takes the form of white spots that are hard to see. In more severe cases (which are rare), the discoloration can be darker, with a pitted texture. The condition is not harmful, but may eventually require cosmetic dental treatment. Tooth decay, on the other hand, is harmful to your child’s health and can also be quite painful in severe cases.
The risk for fluorosis ends by the time a child is about 9 and all the permanent teeth have fully formed. Since fluoride use is cumulative, all the sources your child comes in contact with — including powdered infant formula mixed with fluoridated tap water — need to be evaluated. While caution is advised, however, it would be a mistake to forgo the benefits that this important mineral can bring to your child’s teeth — and his or her overall health.








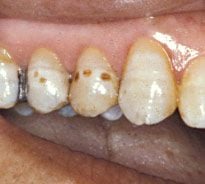 However, there is such a thing as too much fluoride — particularly when it comes to children. If developing teeth absorb too much fluoride, they can become permanently stained or even pitted — a condition referred to as enamel fluorosis. It is not dangerous, but may require cosmetic dental work. That’s why young children should not be allowed to swallow fluoride toothpaste. Adults who take in excessive fluoride throughout their lifetimes may become more prone to bone fractures or tenderness, a condition known as skeletal fluorosis. Severe forms of enamel or skeletal fluorosis are not common in the United States. Still, given that excessive doses of fluoride could cause problems, it’s best to consult a dental professional on the most appropriate products for you and your child to use.
However, there is such a thing as too much fluoride — particularly when it comes to children. If developing teeth absorb too much fluoride, they can become permanently stained or even pitted — a condition referred to as enamel fluorosis. It is not dangerous, but may require cosmetic dental work. That’s why young children should not be allowed to swallow fluoride toothpaste. Adults who take in excessive fluoride throughout their lifetimes may become more prone to bone fractures or tenderness, a condition known as skeletal fluorosis. Severe forms of enamel or skeletal fluorosis are not common in the United States. Still, given that excessive doses of fluoride could cause problems, it’s best to consult a dental professional on the most appropriate products for you and your child to use.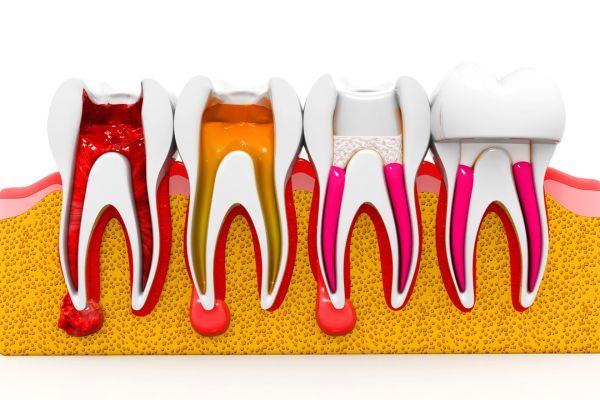


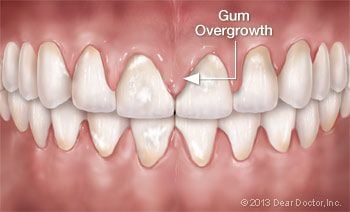 It’s always a good idea to tell your health care providers about any side effects you may be experiencing as soon as you notice them. However, even though gum tissue overgrowth may be a worrisome issue, it doesn’t mean you should stop taking your blood pressure medication! There are several options for controlling this condition, which should be discussed with all members of your medical team.
It’s always a good idea to tell your health care providers about any side effects you may be experiencing as soon as you notice them. However, even though gum tissue overgrowth may be a worrisome issue, it doesn’t mean you should stop taking your blood pressure medication! There are several options for controlling this condition, which should be discussed with all members of your medical team.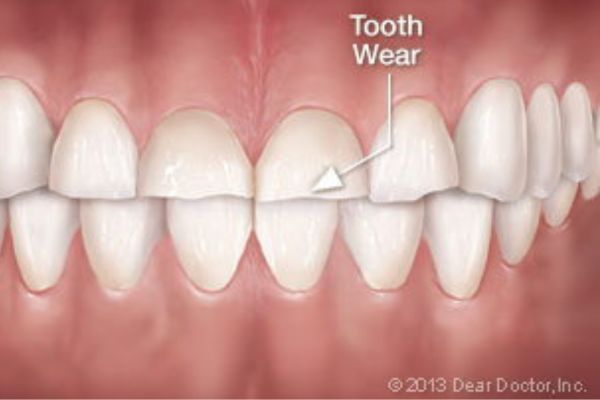
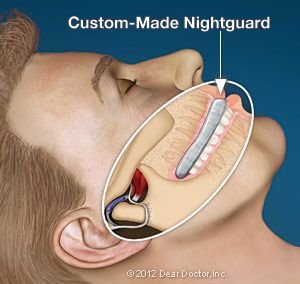 If damage to your teeth or existing dental work is evident, we may recommend a custom-made nightguard, also known as an “occlusal guard,” may be recommended. It resembles an athletic mouthguard. Made of comfortable plastic, the guard is worn at night to keep your teeth from actually contacting each other. It also helps protect your jaw joints from excessive force.
If damage to your teeth or existing dental work is evident, we may recommend a custom-made nightguard, also known as an “occlusal guard,” may be recommended. It resembles an athletic mouthguard. Made of comfortable plastic, the guard is worn at night to keep your teeth from actually contacting each other. It also helps protect your jaw joints from excessive force.

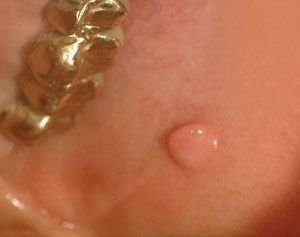 Oral cancer is perhaps the most significant disease to look for in an examination — both because it can be life-threatening, and because early detection is proven to increase the survival rate. But it’s important to remember that a large majority of unusual growths are found to be benign. Some other oral diseases that may be screened for include:
Oral cancer is perhaps the most significant disease to look for in an examination — both because it can be life-threatening, and because early detection is proven to increase the survival rate. But it’s important to remember that a large majority of unusual growths are found to be benign. Some other oral diseases that may be screened for include: