Root Canal Retreatment
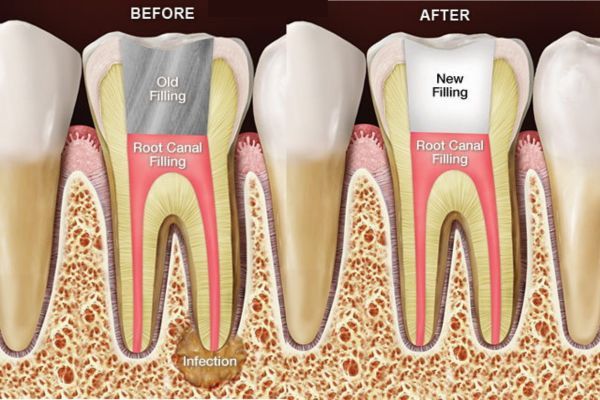
Most of the time, root canal therapy is effective at permanently relieving tooth pain and halting infection of the soft tissues deep inside the teeth and gums. But occasionally, as in any medical procedure, the body may not heal as we expect it to. After a period of time, you may experience pain in the affected tooth again — or, even if you have no symptoms, x-rays may reveal that infection is still present near the tooth’s roots. In that case, you may need root canal retreatment.
There are several reasons why your root canal treatment may not have succeeded at first. The “canals” themselves are slender, forking passageways deep inside the tooth that enclose nerves and blood vessels: the tooth’s soft “pulp.” They can be so narrow and intricate that some may have gone undetected, or failed to respond to treatment the first time. Or, the canals might have become recontaminated via a number of routes: a delayed or ineffective crown restoration, new tooth decay, advancing gum disease, or a cracked or fractured tooth. Any of these conditions could result in reinfection.
If initial root canal (endodontic) therapy has failed, the first thing to do is evaluate your options. Besides retreatment, the alternatives may include endodontic surgery or extraction (removal) of the tooth. However, a missing tooth should be replaced by a dental implant, a bridge or a partial denture as soon as possible — and none of these are simple or inexpensive options. That’s part of the reason we prefer to help you retain your natural teeth whenever possible.
The Retreatment Procedure
If endodontic retreatment is appropriate for you, the procedure is similar to a routine root canal, with a few added measures. After you are anesthetized (usually with a numbing shot), any restorations presently on your tooth — crowns, for example — will be altered to provide access to the root canal filling material. This is usually accomplished by making a small opening into the inner part of the tooth, removing filling material or obstructions, and cleaning the pulp chambers with tiny instruments.
A microscope and light are used to search carefully for additional canals or unusual structures. If the treatment process becomes extremely complex, it may be finished in a subsequent visit. Finally, when all the canals have been cleaned and disinfected, they will be filled with inert material and sealed. Then a temporary filling will be placed in the tooth. A permanent restoration will need to be placed at a later time.
Is Root Canal Retreatment My Best Option?
Medicine and dentistry are as much art as science, and neither one can guarantee that any procedure will be 100% successful. While endodontic retreatment can be more complex than initial root canal therapy, it offers a good chance of success in many instances. And, since the field of endodontics is constantly evolving, it may be possible to use new techniques that weren’t available when your first root canal procedure was done.
Dentists take seriously our responsibility to help you understand the risks, benefits and alternatives for treating root canal problems. When we recommend retreatment, it’s because we feel it is the best way for you to preserve your natural teeth — and we want you to be able to enjoy them for many years to come.