Cosmetic Gum Surgery
Cosmetic gum surgery, or gum contouring, can solve a variety of cosmetic issues relating to the proportions of your teeth and your gums. For example, too much gum tissue may make your teeth appear short, while too little gum tissue will make your teeth appear too long. You may also have a combination of the two, where the tooth to gum ratio varies from tooth to tooth.
Types of Gum Contouring
Gum Reduction Surgery
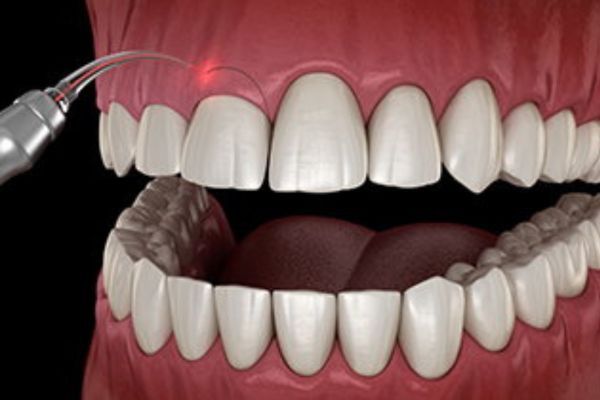
If you have a “gummy smile,” or too much gum tissue covering your teeth, your teeth might appear smaller than you’d like. With the use of a laser or scalpel for soft tissue, your periodontist can remove excess gum tissue to achieve a more proportional smile.
Gum Grafting Surgery
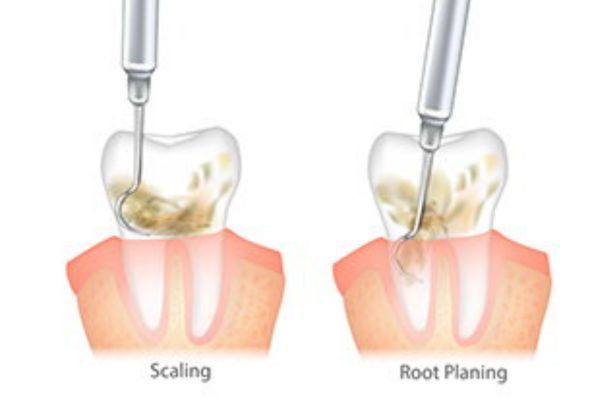
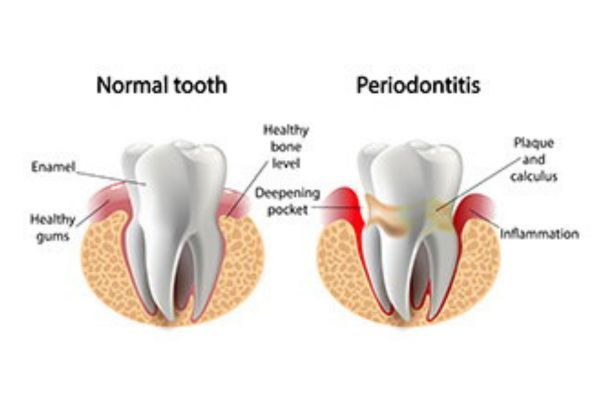
For some people, their gums are either too thin or are receding. Gum recession occurs when the gum tissue pulls away from your teeth, which is typical of an ongoing infection like periodontitis. This pulling away from the teeth not only looks unsightly, but it also creates other oral issues, such as decreased stability and support of the teeth, and exposure of the tooth root. By using tissue elsewhere in your mouth or from a tissue bank, the grafts encourage the recreation of gum tissue. Your teeth will once again have the support they need to remain healthy, as well as the aesthetics you desire.